 The Unreliable
The Unreliable
TSH Lab Test
by Jeffrey Dach MD
Suzy is a 59 year old post menopausal woman with low thyroid function. About three months ago, she started her bio-identical hormone program which included natural thyroid pills. After starting the program, she was doing well with more energy, better sleep, improved appearance of skin and hair, and resolution of her menopausal symptoms of flashes and sweats.
A New Set Of Thyroid Labs
However about 12 weeks into her program, Suzy had a visit with her primary care doctor who did a follow up thyroid panel. Her primary care doctor informed Suzy that her TSH test result was outside of the normal range, and therefore, her thyroid dose was too high, and should be reduced. (Note TSH stands for Thyroid Stimulating Hormone and is made by the pituitary gland)
Too Many Doctors Spoil the Soup
Suzy called me at the office distraught and confused. Two doctors were telling her two different things and she didn't know who to believe. Her primary care doctor was telling her one thing and I was telling her another.
A Low TSH Test is Unreliable For Adjusting Dosage
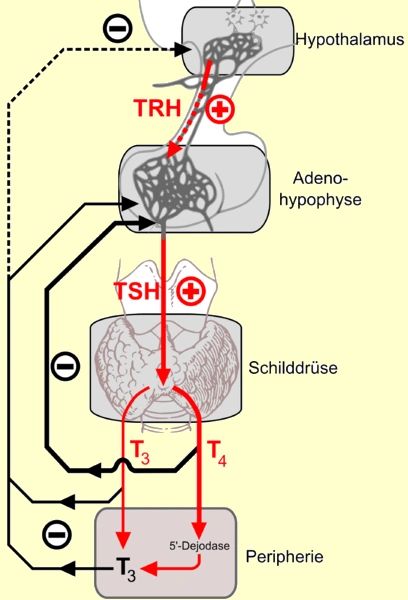 I explained to Suzy that her primary care doctor was incorrect in relying slavishly on the TSH test. Even though her TSH test was 0.15 which is below the lab reference range of 0.3, this was perfectly acceptable and indicated her thyroid medicine was suppressing the TSH to a low level which was perfectly fine.
I explained to Suzy that her primary care doctor was incorrect in relying slavishly on the TSH test. Even though her TSH test was 0.15 which is below the lab reference range of 0.3, this was perfectly acceptable and indicated her thyroid medicine was suppressing the TSH to a low level which was perfectly fine.
No Clinical Evidence of Thyrotoxicosis
I also informed Suzy that her Primary Care Doctor is mistakenly relying on the TSH test to determine her thyroid dosage. The TSH test is an indirect measure of thyroid function and can be unreliable. A more accurate indicator of thyroid function is the free T3, which in her case was 375, well within the normal range of 240 to 420. The Free T3 lab test together with the absence of any signs or symptoms of thyroid excess indicates she is using the correct dosage of natural thyroid medication. Suzy had no symptoms of thyroid excess. The symptoms of thyroid excess include rapid heart beat or palpitations, and Suzy reported no such symptoms. In fact, Suzy said she felt fine and now that she understands it, she didn't want to go back to the way she was feeling before she started the thyroid pills.
This scenario is repeated about once a week at my office.
Conventional Docs Slavishly Rely on the TSH
Conventional primary care doctors use a different lab panel from mine. They never do a Free T3 test which is the most informative thyroid lab test, and instead rely on the TSH which is not a direct measure of thyroid function and can in fact be unreliable. Most conventional doctors are unfamiliar with the use of natural thyroid which contains both T3 and T4, and instead use Synthroid which is quite different, containing only T4.
No Time for Explanations
Since the Primary care doctors bill the health insurance for the office visit and payment is only a few dollars, the office visit is brief, 3-5 minutes. In this short time, Primary care doctors can provide only the most basic care, which is a quick look at the TSH lab test. If the TSH is below the lab reference range the doctor gives a new prescription for Synthroid with a with reduced dosage. If the TSH is above the reference range, the primary care doctor will increase the Synthroid dosage.
The Cleveland Clinic Chimes In
A few months ago, I found myself talking on the phone with an endocrinologist at the Cleveland Clinic explaining why the TSH blood test can be unreliable. He informed me I was wrong, and that he uses the TSH test as the gold standard. We agreed to disagree and parted company as friends. I have found that, in general, endocrinologists and mainstream doctors rely heavily on TSH to make a diagnosis of low thyroid.
Why Thyroid Blood Testing is Unreliable.
 I recommend to you a book
I recommend to you a book
A general practitioner in the British National Health Service, Peatfield came to the US to train at the Broda Barnes Institute. He later returned to England and started his own thyroid clinic. His book contains the wisdom of 25 years of diagnosing and treating thyroid conditions. One section of the book is devoted to the question,
Why are thyroid blood tests unreliable?
Here is what Dr. Peatfield says:
1) Anxiety in the medical establishment about rules and dogma has led to a slavish reliance on blood tests, such as the TSH, which are often unreliable and can actually produce a false picture.2) Very few doctors can accept the fact that a normal, or low TSH, may still occur with low thyroid function.
3) As a result of this test (TSH), thousands are denied treatment for low thyroid condition.
These same sentiments are shared by the teachings of Broda Barnes MD, in his classic book on Low Thyroid. Broda Barnes MD reported 40 years ago on the same problems with his medical colleagues relying too heavily on thyroid blood tests.

Broda Barnes estimated that up to 40% of the population suffers from a low thyroid condition and would benefit from thyroid medication. Of course, Barnes' opinion differed with that of mainstream medicine of his time which relied dogmatically on thyroid blood tests to make the diagnosis of low thyroid. Barnes felt the blood tests were unreliable and instead used the basal temperature, history and physical examination. This medical debate regarding unreliability of thyroid blood testing continues today.
Being an astute clinician, Dr. Barnes makes a number of observations about the low thyroid condition. Firstly, low thyroid is associated with a reduced immunity to infectious diseases such as TB. Before the advent of modern antibiotics in the 1940's, most low thyroid children succumbed to infectious diseases before reaching adulthood. Secondly, low thyroid is associated with a peculiar form of skin thickening called myxedema which causes a characteristic appearance of the face, puffiness around the eyes, fullness under the chin, loss of outer eyebrows, and hair thinning or hair loss.
A third observation by Dr. Barnes is that low thyroid is associated with menstrual irregularties, miscarriages and infertility. Barnes treated thousands of young women with thyroid which restored cycle regularity and fertility. In his day, the medical system resorted to the drastic measure of hysterectomy for uncontrolled menstrual bleeding. Although today's use of birth control pills to regulate the cycles is admittedly a far better alternative, Barnes found that the simple administration of desiccated thyroid served quite well. Again, Barnes noted that blood testing was usually normal in these cases which respond to thyroid medication.
A lengthy chapter is devoted to heart attacks and the low thyroid condition. Based on autopsy data from Graz Austria, Barnes concluded that low thyroid patients who previously would have succumbed to infectious diseases in childhood go on years later to develop heart disease. Barnes also found that thyroid treatment was protective in preventing heart attacks, based on his own clinical experience. Likewise for diabetes, Dr. Barnes found that adding thyroid medication was beneficial at preventing the onset of vascular disease in diabetics. Again, blood tests are usually normal.
Dr. Barnes devotes separate chapters in the book to discussion of chronic fatigue, migraine headaches and emotional/behavioral disorders all of which respond to treatment with thyroid medication.
The final chapter describes Dr. Barnes work on obesity when he resided over a hospital ward of volunteer obese patients, and monitored everything they ate. He found that the obese patients invariably ate a high carbohydrate diet, and avoided fat. Barnes added fat back into the menu and reduced the refined carbohydrates and found that his obese patients lost 10 pounds a month with no hunger pangs.
Missing from the book are discussions of Iodine supplementation and the role of the Adrenal, both of which are covered in later updated versions of Barnes thyroid book by other authors.
See
Iodine supplementation is covered by both Derry and Brownstein. The Safe Uses of Cortisol by William McK Jefferies is the companion medical classic devoted to the adrenals and cortisol.
Broda Barnes Institute
Although Broda Barnes has since passed away, his work lives in at the Broda Barnes Institute. Patricia Puglio is the director and a great resource. She is available by phone to answer questions and offer suggestions. Here is her contact information:
Patricia A. Puglio, Director, Broda O. Barnes, M.D. Research Foundation, Inc. PO Box 110098 Trumbull, CT 06611 phone (203) 261-2101 www.brodabarnes.org
Articles With Related Content:
Reasons Why Thyroid Testing Can Be Unreliable
Hunt Study Shows Thyroid Prevents Heart Attacks
More Thyroid Articles
Jeffrey Dach MD
7450 Griffin Rd Suite 180/190
Davie, FL 33314
Phone: 954-792-4663
Blog
Links and References
http://www.altsupportthyroid.org/tsh/tshmedrefs5.php
http://www.altsupportthyroid.org/tsh/tshmedrefs5.php
Suppressed TSH Levels: Medical Journals
http://www.altsupportthyroid.org/tsh/tshexp1pr.php
TSH and Patients' Experiences: Suppressed to 0.5
http://ccpd.ucsf.edu/hypothyroidism.shtml
Hypothyroidism (Thyroid Hormone Deficiency) UCSF Pituitary Disorders
TSH is often an unreliable measure of secondary hypothyroidism and should not be used to assess the adequacy of thyroid replacement in these patients. The inappropriate use of TSH levels to determine hormone replacement is one of the more common mistakes that we see in the patients we follow, and patients should be cautious if another physician discusses changing their thyroid hormone dose. Many patients have returned for their one-year follow-up visits having had their doses lowered in response to "low TSH levels." Most of them feel poorly, but improve after we increase or restart their medication.
http://www.bmj.com/cgi/content/full/326/7398/1087
BMJ 2003;326:1087 (17 May), doi:10.1136/bmj.326.7398.1087
Letter- Thyroid function tests and hypothyroidism
In the Framingham study a low serum thyroid stimulating hormone concentration was shown to be a risk factor for the development of atrial fibrillation,1 but the patients in question were a heterogeneous group, the minority of whom were taking thyroxine. A similarly misleading conclusion has been drawn from the recent Birmingham study in which a low serum thyroid stimulating hormone (< 0.5 mU/l) was associated with an increase in cardiovascular mortality.2
This finding has been used to argue that a suppressed serum concentration of thyroid stimulating hormone should be avoided in patients taking thyroxine replacement,3 although thyroxine treatment was one of the exclusion criteria. The weakness of the meta-analysis, showing that thyroxine induced suppression of thyroid stimulating hormone led to reduced bone mineral density, was recognised by the authors themselves, who said that their design (cross sectional studies) was not appropriate because the many risk factors for bone loss do not allow correct matching of controls with cases.4 This realistic assessment accords with the earlier views of Franklyn et al that thyroxine treatment alone does not represent a significant risk factor for loss of bone mineral density.5
We have long taken the view that most hypothyroid patients are content with a dose of thyroxine that restores serum concentrations of thyroid stimulating hormone to the low normal range. However, some achieve a sense of wellbeing only when serum thyroid stimulating hormone is suppressed, when we take care to ensure that serum tri-iodothyronine is unequivocally normal.
Until valid evidence shows that such a policy is detrimental we will continue to treat patients holistically rather than insist on adherence to a biochemical definition of adequacy of thyroxine replacement. The issue of whether a little too much thyroxine is dangerous is likely to evaporate when appropriate preparations become available to allow treatment of hypothyroidism with both tri-iodothyronine and thyroxine.
A D Toft, consultant physician - Endocrine Department Royal Infirmary of Edinburgh, Edinburgh EH3 9YW G J Beckett, reader University Department of Clinical Biochemistry Royal Infirmary of Edinburgh, Edinburgh EH3 9YW
References: Sawin CT, Geller A, Wolf PA, Belanger AJ, Baker E, Bacharach P, et al. Low serum thyrotropin concentrations as a risk factor for atrial fibrillation in older persons. N Engl J Med 1994;331: 1249-52.[Abstract/Free Full Text]
Parle JV, Maisonneuve P, Sheppard MC, Boyle P, Franklyn JA. Prediction of all-cause and cardiovascular mortality in elderly people from one low serum thyrotropin result: a 10-year cohort study. Lancet 2001;358: 861-5.
Fatourechi V. Adverse effects of subclinical hyperthyroidism. Lancet 2001;358: 861-5.
Uzzan B, Campos J, Cucherat M, Nony P, Boissel JP, Perret GY. Effects on bone mass of long term treatment with thyroid hormones: a meta-analysis. J Clin Endocrinol Metab 1996;81: 4278-89.[Abstract]
Franklyn J, Betteridge J, Holder R, Daykin J, Lilley J, Sheppard M. Bone mineral density in thyroxine treated females with or without a previous history of thyrotoxicosis. Clin Endocrinol 1994;41: 425-32.[Medline]
http://www.ncbi.nlm.nih.gov/pubmed/4062219?dopt=Abstract
Ann Clin Biochem. 1985 Sep;22 ( Pt 5):506-8.Related Articles, Links
Clinical value of a sensitive immunoradiometric assay for TSH.
Allen KR, Scott RD, Hewitt JV, Watson D.
We have investigated a sensitive immunoradiometric assay for serum thyroid-stimulating hormone (TSH) in 45 thyrotoxic patients not on treatment, 464 euthyroid patients and 111 hypothyroid patients on replacement therapy. Forty-three thyrotoxic and seven euthyroid patients were found to have an undetectable TSH (less than 0.2 mIU/L). Previous work has shown a very clear separation of thyrotoxic and euthyroid patients using sensitive TSH assays. However, our extended study here has revealed that a significant number of euthyroid patients with undetectable TSH (1.5% in our study) are likely to be found if TSH becomes the initial test for thyroid function. Thirty of the hypothyroid patients on thyroxine were found to have undetectable TSH, but only one showed clinical signs of thyrotoxicosis. Most of the patients, although having raised serum free T4, had serum free T3 levels within the euthyroid range or just slightly elevated.
Jeffrey Dach MD
7450 Griffin Road Suite 190
Davie, Florida 33314
954-792-4663
http://www.jeffreydachmd.com
http://www.drdach.com/
http://www.naturalmedicine101.com/
http://www.truemedmd.com/
http://www.bioidenticalhormones101.com/
For Disclaimer: Click Here
The reader is advised to discuss the comments on these pages with
his/her personal physicians and to only act upon the advice of his/her
personal physician. Also note that concerning an answer which appears as
an electronically posted question, I am NOT creating a physician —
patient relationship.
Although identities will remain confidential as much as possible, as I can not control the media, I can not take responsibility for any breaches of confidentiality that may occur.
Copyright (c) 2014 Jeffrey Dach MD All Rights Reserved
This article may be reproduced on the internet without permission,
provided there is a link to this page and proper credit is given.
FAIR USE NOTICE: This site contains copyrighted material the use of which has not always been specifically authorized by the copyright owner. We are making such material available in our efforts to advance understanding of issues of significance. We believe this constitutes a ‘fair use’ of any such copyrighted material as provided for in section 107 of the US Copyright Law. In accordance with Title 17 U.S.C. Section 107, the material on this site is distributed without profit to those who have expressed a prior interest in receiving the included information for research and educational purposes.
Serving Areas of: Hollywood, Aventura, Miami, Fort Lauderdale, Pembroke Pines, Miramar, Davie, Coral Springs, Cooper City, Sunshine Ranches, Hallandale, Surfside, Miami Beach, Sunny Isles, Normandy Isles, Coral Gables, Hialeah, Golden Beach ,Kendall,sunrise, coral springs, parkland,pompano, boca raton, palm beach, weston, dania beach, tamarac, oakland park, boynton beach, delray,lake worth,wellington,plantation
.