 Low Testosterone From Pain Pills
Low Testosterone From Pain Pills
by Jeffrey Dach MD
Joe has chronic fatigue, weakness, and erectile dysfunction. He was doing well until 10 years ago when he started pain pills after a car accident which left him with chronic back pain.
Left image: poppy field in Burma courtesy of wikimedia commons. Poppies are source for opium, a narcotic pain medication.
Chronic Pain Treated with Opioid Narcotics
After the car accident, Joe's family doctor prescribed oxycontin pain pills, hoping the chronic back pain would eventually get better. Unfortunately, Joe's back pain did not get better, and he still takes pain pills every day. Even though the pain pills are no longer effective, Joe finds it nearly impossible to get off them because of the severe withdrawal effects.
 Low Testosterone Detected on Blood Tests
Low Testosterone Detected on Blood Tests
Joe's lab testing showed very low testosterone levels. This explained the fatigue, weakness and low libido. Joe was started on bioidentical testosterone as a topical gel, and 6 weeks later he reports that his fatigue and weakness is gone, and his wife is much happier with his renewed libido. Joe also noticed his chronic pain seemed to decrease in intensity, and he was now interested in pursuing the idea of tapering off the narcotic pain pills.(4)
Above Left image: Synthetic opiate hydrocodone (Vicodin Tablet) courtesy of wikimedia commons. Vicodin Tablet is chemically altered version of Opium Poppy.
Doctors Freely Prescribe Narcotic Pain Pills
When patients like Joe seek help from their doctor for a painful condition, they will be given narcotic pain tablets such as percocet, oxycodone, roxycodone and oxycontin. These pain pills are quite effective at relieving the painful condition. However, they come with severe adverse side effects.
 Adverse Effects of Long Term Pain Pills (Opiates)
Adverse Effects of Long Term Pain Pills (Opiates)
We all know that Pain Pills, such as opioid narcotics, are highly addictive and come with severe adverse effects. Opiate containing narcotic Pain Pills were never intended for long term use. They cause profound suppression of the endocrine system, and in men, profound inhibition of testosterone production. This type of low testosterone is quite common, and yet, may go unrecognized by the busy primary care doctor. (1)
Another adverse effect of long-term opioid use is opioid-induced hyperalgesia. This is a form of hypersensitivity to pain. The original painful condition becomes worse. Other adverse effects include impaired cognitive function, and suppression of the immune system with tendency to develop infection.(6)
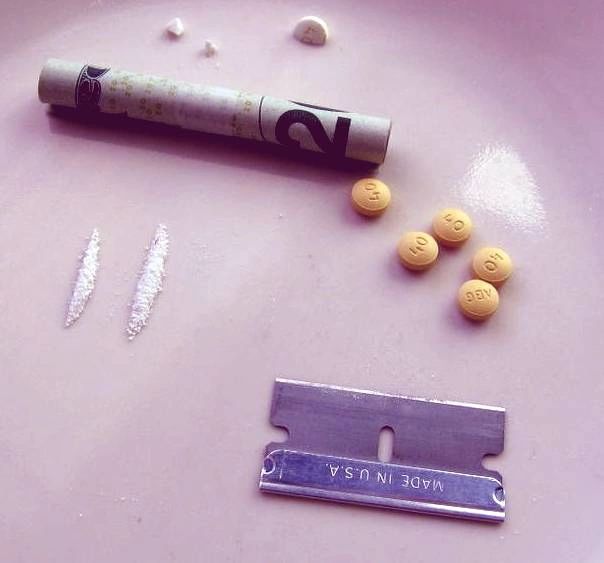
Above image: OxyContin tablets crushed into powder for insufflation (snorting). Notice the tablets at the top with the coating removed. The tablets are distributed by AB Generics, hence the ABG stamp on the back. Image Courtesy of wikimedia commons. Oxycontin is chemically altered version of opium poppy.
 Chronic Opioid Pain Pills Lose Effectiveness Long Term
Chronic Opioid Pain Pills Lose Effectiveness Long Term
Another problem with long term use of narcotic pain pills, is that they lose their effectiveness over time. The brain and nervous system develops a "tolerance" to the drug, and higher doses are required to achieve the same result.(7) The initial pain relief from opioid pain pills may not be sustained long term because of drug tolerance, opioid-induced hyperalgesia, and intermittent drug withdrawal effects. (7) In other words the pills lose their effectiveness, and yet continue to produce dependence and adverse effects.
Left image: Young drug addict injecting narcotic opiate drug into left arm. Heroin is chemically altered version of Opium Poppy. Courtesy of wikimedia commons.
Low Testosterone Goes Largely Unrecognized
Although quite common, Opioid-induced androgen deficiency and has gone largely unrecognized by the medical community(1). Low testosterone is caused by opioid drug inhibition of LH (Leutininizing Hormone), a pituitary hormone involved in testosterone production, as well direct inhibition of testosterone itself. Similarly, there is also inhibition of the entire endocrine system, and adrenal hormone suppression.
Symptoms of low testosterone include fatigue, depression, hot flashes, night sweats, diminished libido, erectile dysfunction, and diminished sexual arousal and satisfaction. Men may also develop osteoporosis, anemia, and diminished muscle mass. (2)(3) Women who consume opioid-pain pills will stop having menstrual cycles and will notice greatly diminished libido (sex drive). (5)

Left Image
opium poppy courtesy of wikimedia commons. This plant is used to make
opium, a natural source for narcotic pain medication. Courtesy of
wikimedia commons.
Testosterone Treatment Effective and Recommended by Mainstream Medicine
Administration of topical testosterone, or injectable testosterone has been studied and found effective for men with low testosterone on pain pills. (4)
Our Approach to Evaluation and Treatment
For men with a chronic pain condition who have been on long-term pain pills, our evaluation includes a complete blood testing panel looking for vitamin, mineral and nutritional deficiencies. We find these deficiencies quite commonly in this group. In addition, evaluation includes a complete hormone panel looking at the entire endocrine system, and adrenal function. If extensive testing shows low hormone levels, then hormone supplementation is offered.
 Opiate Detoxification Program is Essential
Opiate Detoxification Program is Essential
The reality is that hormone supplementation and nutritional supplementation for the long term opiate pain pill user is only a temporary bandaid. To fully restore health, the opiate addiction must be addressed and the patient must ultimately get off the pain pills. This may be difficult to do on their own because of severe drug withdrawal symptoms. Therefore, we provide the patient with a referral to any one of a number of doctors who specialize in narcotics detoxification, and urge the patient to strongly consider this option.
Above left image: 2D structure of synthetic opiate hydrocodone (Vicodin) courtesy of wikimedia commons.
Rick Sponaugle MD
One such specialist is Rick Sponaugle MD at the Florida Detox Center. Dr Sponaugle is board certified in anesthesiology and addiction medicine. Dr Sponaugle's facility offers a painless and rapid detox program, utilizing general anesthesia and sophisticated intra-operative monitoring of the brain and cardiovascular system. In addition, the center offers other programs for detox from alcohol and benzodiazepine addiction.
Contact Information:
Rick Sponaugle MD at the Florida Detox Center
Florida Detox® & Wellness Institute
32815 US Highway 19 N
Palm Harbor, FL 34684
Toll-free: 1-888-775-2770
Jeffrey Dach MD
7450 Griffin Rd Suite 180/190
Davie, FL 33314
Phone: 954-792-4663
Facebook
Blog
Articles with related content
Low Testosterone Could Be Killling You
John Crisler on HCG
Benefits of Testosterone Part One
Benefits of Testosterone Part Two
Links and References
(1) http://journals.lww.com/co-endocrinology/
Abstract/2006/06000/Opioid_induced_androgen_deficiency.6.aspx
Current Opinion in Endocrinology and Diabetes: June 2006 - Volume 13 - Issue 3 - p 262-266 . Opioid-induced androgen deficiency by Daniell, Harry W
Opioid-induced androgen deficiency has become one of the most common causes of testosterone deficiency among men in many communities. Its increase parallels the large increase in opioid use. This form of hypogonadotrophic hypogonadism is present in most men chronically consuming sustained-action opioids, including those receiving methadone for heroin addiction and those consuming opioids for control of either malignant or non-malignant chronic pain. A similar, but less well defined illness occurs in women. Opioid-induced androgen deficiency is not widely recognized. This review examines its pathophysiology, some of its signs and symptoms, and indicates some areas where current observations suggest additional investigations would be fruitful.
Recent findings: Recognition of opioid-induced androgen deficiency in men not receiving methadone for heroin addiction is a new observation, and in these men contributes to fatigue, depression, vasomotor phenomena, anemia, diminished libido, erectile dysfunction and osteoporosis. These signs and symptoms improved during testosterone replacement therapy in several small non-placebo-controlled trials.
Summary: A large majority of men consuming sustained-action opioids have symptomatic androgen deficiency which apparently responds to replacement therapy. Opioid-induced androgen deficiency is frequently overlooked, with its symptoms attributed to underlying disease states including malignant disease, chronic back disorders, HIV disease, and psychosocial illnesses contributing to opioid habituation.
(2) http://www.amjmed.com/article/S0002-9343(06)00614-0/fulltext
Volume 120, Issue 9, Page e21 (September 2007)
Opioid-induced Androgen Deficiency Discussion in Opioid Contracts Harry W. Daniell, MD
Strong inhibition of androgen production quickly follows the onset of sustained-action opioid use, whether the opioids are administered orally,2, 3, 4, 5 transdermally,4 or intrathecally.3, 5, 6, 7, 8 These low androgen levels result in classic symptoms of hypogonadism in a majority of opioid-consuming men, with most of them exhibiting various combinations of fatigue, depression, hot flashes, night sweats, diminished libido, erectile dysfunction, and diminished sexual arousal and satisfaction. Low androgen levels also contribute to physical changes, including osteoporosis, anemia, and diminished muscle mass. Similar changes occur in opioid-consuming premenopausal women, most of whom demonstrate amenorrhea or anovulatory menstrual cycles soon after beginning sustained-action opioid use.6, 8, 9, 10 Most premenopausal and postmenopausal women also demonstrate greatly diminished libido 6, 8, 10 at this time.
Signs and symptoms of hypogonadism typically improve in men with OPIAD during replacement testosterone therapy4 and in the few women who have received hormone replacement therapy for opioid-related symptoms of hormone deficiency.6, 10
In my private practice of general internal medicine, the discussion of OPIAD in our opioid contracts includes the potential usefulness of replacement hormonal therapy and potential complications of this therapy. We have found this information to be of help in establishing the patient-physician partnership described and recommended by Arnold et al,1 which clearly is required for optimal chronic use of opioids. As part of this information exchange, we obtain sex-hormone levels in all outpatients about to begin chronic sustained-action opioid therapy and again with the development of symptoms of hypogonadism.
(3) http://www.jpain.org/article/S1526-5900(02)00032-9/abstract?refuid=S0002-9343(06)00614-0&refissn=0002-9343
Hypogonadism in men consuming sustained-action oral opioids
Presented in part at the 16th Annual Meeting of the Society for Ambulatory Anesthesia, Palm Springs, CA, May 2-5, 2001. Harry W. Daniell Volume 3, Issue 5, Pages 377-384 (October 2002)
Naturally occurring opiates (endorphins) diminish testosterone levels by inhibiting both hypothalamic gonadotrophin releasing hormone production and testicular testosterone synthesis. Heroin addicts treated with a single daily dose of methadone and nonaddicts receiving continuous intrathecal opioids quickly develop low luteinizing hormone and total testosterone levels. A similar pattern was sought in men consuming commonly prescribed oral opioids. Free testosterone (FT), total testosterone (TT), estradiol (E2), dihydrotestosterone (DHT), luteinizing hormone (LH), and follicle-stimulating hormone (FSH) were measured in 54 community-dwelling outpatient men consuming oral sustained-action dosage forms of opioids several times daily for control of nonmalignant pain. Hormone levels were related to the opioid consumed, dosage and dosage form, nonopioid medication use, and several personal characteristics and were compared with the hormone analyses of 27 similar men consuming no opioids.
Hormone levels averaged much lower in opioid users than in control subjects in a dose-related pattern (P < .0001 for all comparisons). FT, TT, and E2 levels were subnormal in 56%, 74%, and 74%, respectively, of opioid consumers. Forty-eight men (89%) exhibited subnormal levels of either FT or E2. Either TT or E2 level was subnormal in all 28 men consuming the equivalent of 100 mg of methadone daily and in 19 of 26 (73%) consuming smaller opioid doses. Eighty-seven percent (39 of 45) of opioid-ingesting men who reported normal erectile function before opioid use reported severe erectile dysfunction or diminished libido after beginning their opioid therapy. Commonly prescribed opioids in sustained-action dosage forms usually produce subnormal sex hormone levels, which may contribute to a diminished quality of life for many patients with painful chronic illness.
(4) http://www.ncbi.nlm.nih.gov/pubmed/16516826
J Pain. 2006 Mar;7(3):200-10.
Open-label pilot study of testosterone patch therapy in men with opioid-induced androgen deficiency. Daniell HW, Lentz R, Mazer NA. Department of Family Practice, University of California Davis Medical School, Redding, California, USA.
We conducted a 24-week open-label pilot study of testosterone (T) patch therapy in 23 men with opioid-induced androgen deficiency (OPIAD). The T dosage was 5 mg/day for the first 12 weeks and 7.5 mg/day for the second 12 weeks. Seven subjects discontinued prematurely: 4 for noncompliance, 2 for skin irritation and 1 for hepatitis C treatment. In the "completers" population (n = 16), mean (SD) free T levels (normal range 52 to 280 pg/mL) were 28.5 (18.6) pg/mL at baseline, 72.8 (29.6) pg/mL on 5 mg/day (P < .001 vs. baseline), and 120.2 (69.5) pg/mL on 7.5 mg/day (P < .001 vs. baseline and P < .01 vs. 5 mg/day). Total T, dihydrotestosterone, and estradiol showed parallel changes. Sex hormone-binding globulin levels were elevated at baseline and decreased modestly with treatment (P < .05 vs. baseline at 5 mg/day; P < .01 vs. baseline at 7.5 mg/day). Luteinizing hormone levels were in the low-normal range at baseline and suppressed markedly with treatment (P < .001 vs. baseline at both doses). Androgen deficiency symptoms (ADSQ), sexual function (Watts SFQ), mood (PGW, depression (BDI-II), and hematocrit levels showed improvement during treatment, generally more so at the 7.5 mg/day dosage (P < .001 vs. baseline for most parameters). Pain scores (BPI-SF) decreased slightly on 7.5 mg/day (interference score: P < .05 vs. baseline and 5 mg/day); the use of opioids did not change appreciably. The testosterone patches were generally well tolerated.
PERSPECTIVE: Long-acting opioid preparations suppress the hypothalamic-pituitary-gonadal axis in men and produce a symptomatic state of opioid-induced androgen deficiency (OPIAD). Testosterone patch therapy at a dose of 7.5 mg/day normalizes hormone levels and appears to improve a number of quality of life parameters (eg, sexual function, well-being, mood) in men with OPIAD.
(5) http://www.ncbi.nlm.nih.gov/pubmed/17936076
J Pain. 2008 Jan;9(1):28-36. Epub 2007 Nov 1.
Opioid endocrinopathy in women consuming prescribed sustained-action opioids for control of nonmalignant pain. Daniell HW. Department of Family Practice, University of California Davis Medical School, Redding, California, USA.
Hypogonadotrophic hypogonadism is characteristically induced in men by intrathecal, transdermal, or sustained-action opioids. Although women receiving intrathecal opioids have similar changes, often accompanied by amenorrhea, hypogonadotrophic hypogonadism has not been documented in women receiving sustained-action, transdermal, or oral opioids. Dehydroepiandrosterone sulfate deficiency, indicating adrenal inhibition, is present in most men and women chronically consuming sustained-action oral or transdermal opioids.
We recorded menstrual histories and measured gonadotrophin, androgen, and estradiol levels in 47 women ages 30 to 75 years who were consuming sustained-action oral or transdermal opioids for control of nonmalignant pain and in 68 non-opioid-consuming control subjects.
Testosterone, estradiol, and dehydroepiandrosterone sulfate values were 48% to 57% lower in opioid-consuming women with intact ovarian tissue than in control subjects (P < .01-.05). Luteinizing hormone and follicle-stimulating hormone values averaged 30% lower in premenopausal and 70% lower in postmenopausal opioid consumers (P < .001).
Among oophorectomized women not consuming estrogen, free testosterone levels were 39% lower in opioid consumers (P < .05), indicating impaired adrenal androgen production. Additional lowering of free testosterone levels was associated independently with oral estrogen replacement and low body mass index. Menses had often ceased soon after beginning sustained-action opioid therapy.
Our observations document hypogonadotrophic hypogonadism plus decreased adrenal androgen production in most women consuming sustained-action oral or transdermal opioids.
PERSPECTIVE: These observations demonstrate profound inhibition of ovarian sex hormone and adrenal androgen production among women chronically consuming sustained-action opioids. Related consequences include altered menstrual flow, probable reduced fertility, and possible contributions to opioid-associated depression, osteoporosis, and hyperalgesia. Measurements of bone density, estradiol, and free testosterone may guide appropriate therapy.
(6) http://www.ncbi.nlm.nih.gov/pubmed/17873598
Curr Opin Anaesthesiol. 2007 Oct;20(5):451-5.
An update on the role of opioids in the management of chronic pain of nonmalignant origin. Højsted J, Sjøgren P. Multidisciplinary Pain Center, Rigshospitalet, Blegdamsvej 9, 2100 Copenhagen Ø, Denmark.
PURPOSE OF REVIEW: To summarize and reflect over primarily recent epidemiological and randomized controlled trials in opioid-treated chronic nonmalignant pain patients, focusing on effects, side effects, risks and long-term consequences of the treatment.
RECENT FINDINGS: In the western world opioids are increasingly being used for long-term treatment of chronic nonmalignant pain. While the long-term benefits of opioids regarding pain relief, functional capacity and health-related quality of life still remain to be proven, studies are emerging that describe serious long-term consequences such as addiction, opioid-induced hyperalgesia, cognitive disorders, and suppression of the immune and reproductive systems.
SUMMARY: Much more research is needed concerning long-time effects and consequences of opioid therapy in chronic nonmalignant pain patients; however, some clear warning signals have been sent out within recent years.
(7) http://www.ncbi.nlm.nih.gov/pubmed/18574357
Clin J Pain. 2008 Jul-Aug;24(6):469-78.
Efficacy of opioids for chronic pain: a review of the evidence. Ballantyne JC, Shin NS.Division of Pain Medicine, Massachusetts General Hospital, Boston, MA 02114, USA.
Opioid therapy for chronic pain has been popularized over the past few decades, and a concern has arisen that the analgesic efficacy of opioids is not always maintained over prolonged courses of treatment despite dose escalation and stable pain. Considering the potentially serious adverse effects of opioids, the idea that pain relief could diminish over time may have a significant impact on the decision to embark on this therapy, especially in vulnerable individuals. Possible loss of analgesic efficacy is especially concerning, considering that dependence may make it hard to withdraw opioid therapy even in the face of poor analgesia. This article first reviews the evidence on opioid efficacy when used for the treatment of chronic pain, and concludes that existing evidence suggests that analgesic efficacy, although initially good, is not always sustained during continuous and long-term opioid therapy (months to years). The theoretical basis for loss of analgesic efficacy over time is then examined. Mechanisms for loss of analgesic efficacy proposed are pharmacologic tolerance, opioid-induced hyperalgesia, subtle and intermittent withdrawal, and a number of psychologic factors including loss of the placebo component.
http://www.viamedica.pl/gazety/gazetaE/darmowy_pdf.phtml?indeks=33&indeks_art=263 Zbigniew Zylicz
Consultant in Palliative Medicine, Dove House Hospice, Hull, United Kingdom
Opioid-induced hypogonadism: the role of androgens in the well-being and pain thresholds in men and women with advanced disease
http://jcem.endojournals.org/cgi/content/full/85/6/2215
Endocrine Consequences of Long-Term Intrathecal Administration of Opioids
Roger Abs, Johan Verhelst, Jan Maeyaert, Jean-Pierre Van Buyten, Frank Opsomer, Hugo Adriaensen, Jan Verlooy, Tony Van Havenbergh, Mike Smet and Kristien Van Acker The Journal of Clinical Endocrinology & Metabolism Vol. 85, No. 6 2215-2222 Jeffrey Dach MD
Disclaimer click here: http://www.drdach.com/wst_page20.html
Although identities will remain confidential as much as possible, as I
can not control the media, I can not take responsibility for any
breaches of confidentiality that may occur.
Copyright (c) 2014 Jeffrey Dach MD All Rights Reserved
FAIR USE NOTICE: This site contains copyrighted material the use of
which has not always been specifically authorized by the copyright
owner. We are making such material available in our efforts to advance
understanding of issues of significance. We believe this constitutes a
‘fair use’ of any such copyrighted material as provided for in section
107 of the US Copyright Law. In accordance with Title 17 U.S.C. Section
107, the material on this site is distributed without profit to those
who have expressed a prior interest in receiving the included
information for research and educational purposes.
Serving Areas of: Hollywood, Aventura, Miami, Fort Lauderdale,
Pembroke Pines, Miramar, Davie, Coral Springs, Cooper City, Sunshine
Ranches, Hallandale, Surfside, Miami Beach, Sunny Isles, Normandy Isles,
Coral Gables, Hialeah, Golden Beach ,Kendall,sunrise, coral springs,
parkland,pompano, boca raton, palm beach, weston, dania beach, tamarac,
oakland park, boynton beach, delray,lake worth,wellington,plantation.
In conclusion, of all patients receiving intrathecal opioids, the large majority of men and all women developed hypogonadotropic hypogonadism, about 15% developed central hypocorticism, and about 15% developed GH deficiency. These findings suggest that further investigations are required to determine the need for systematic endocrine work-up in these patients and the necessity for substitutive therapy.
7450 Griffin Road Suite 190
Davie, Florida 33314
954-792-4663
http://www.drdach.com/
http://www.naturalmedicine101.com/
http://www.truemedmd.com/
http://www.bioidenticalhormones101.com/
The reader is advised to discuss the comments on these pages with
his/her personal physicians and to only act upon the advice of his/her
personal physician. Also note that concerning an answer which appears as
an electronically posted question, I am NOT creating a physician —
patient relationship.
This article may be reproduced on the internet without permission,
provided there is a link to this page and proper credit is given.